Think of the impact wearable devices could have on the millions of people managing chronic diseases through decreased costs and improved outcomes – as well…


Think of the impact wearable devices could have on the millions of people managing chronic diseases through decreased costs and improved outcomes – as well…

At this week’s HIMSS Patient Engagement Summit, getting patients actively involved in their care will be explored as “the blockbuster drug of the 21st Century.”…
Proteus Duxbury, the CTO of Connect for Health Colorado, discusses the steps taken to establish Colorado’s state insurance exchange network and the added challenge of…

Get Ready for Digital Therapeutics Omada Health predicts it is ushering in a new era of medicine called “digital therapeutics.” Digital therapeutics is based on…

Industrial designer Marc Harrison suffered a brain injury while sledding when he was 11-years old. The injury and years of rehabilitation would provide Harrison with…
The iWatch will allow Apple to monetize the immediate context and environment and allow it to amass a wealth of data on both your bodily…
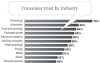
It’s amazing how many companies forget trust when it comes to platforms, networks and user data, but it is fundamental. Facebook and Google may use…

Interactivity, and not just technological interactivity, may be the secret to getting patients engaged. Doing is infinitely more interesting than being talked at or just…
As we move toward digital health and digital payments, the relationships between spending, environment, and other health determinants are becoming clearer, including the choices we…
Engaged patients have better outcomes and cost less to care for. How do we get patients who are not engaged to become more participatory?

